Pain Relief for short-stay procedures
SMS eScript tokenMost patients go home with an SMS eScript token (a QR code or link) on their phone.
How to use it
• Show the token to any pharmacy
• Keep it private (do not share screenshots)
• You can ask the price before the medicine is dispensed
• Some medicines (Schedule 8 strong pain medicines) require ID
Typical medicines after surgery
Pain is usually managed with a layered approach:
• regular paracetamol
• an anti-inflammatory if it is safe for you
• a small amount of stronger pain medicine if needed
Good pain control helps recovery. It allows you to breathe deeply, move earlier and reduces complications such as chest infections and blood clots.
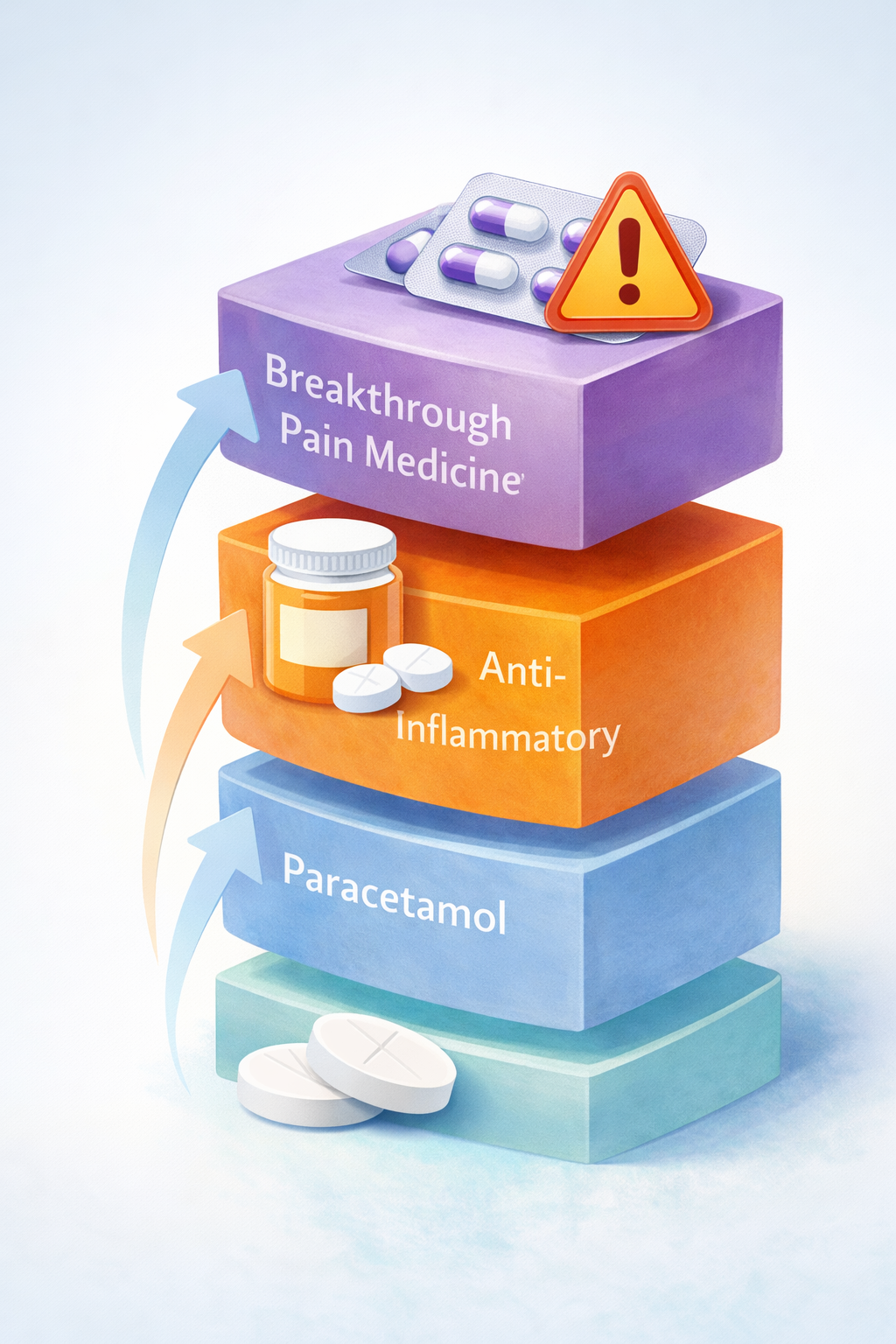
Pain relief ladder
Regular paracetamol
Anti-inflammatory (etoricoxib, celecoxib or ibuprofen)
Stronger medicine only if needed
Pain relief at homePain relief at home uses a layered approach. Start with regular medicines and add stronger medicine only if needed.
Paracetamol
Take regularly for the first 7–14 days (e.g. 2 tablets three times daily). Maximum 6 tablets in 24 hours. Do not take other medicines containing paracetamol (such as cold/flu tablets or Panadeine).
Anti-inflammatory medicine
If prescribed, do not take other anti-inflammatory medicines (ibuprofen, naproxen, diclofenac) at the same time unless advised. Avoid if you have kidney disease, stomach ulcers or are on blood thinners unless approved. Stop and seek advice if you develop indigestion or black stools.
Breakthrough pain medicine
Use only if pain is not controlled by the medicines above. Side effects may include drowsiness, nausea and constipation. Maintain fluids and fibre, and ask a pharmacist or doctor about laxatives if needed.
Safety and recovery
• Do not drive or operate machinery if drowsy. Alcohol increases risk.
• Use ice for 15–20 minutes and elevate the leg to reduce swelling.
Seek medical advice if pain worsens or is not controlled, or if you develop fever, increasing redness or swelling, calf pain or swelling, chest pain or shortness of breath.
When to reduce the medicinesStart reducing your pain medicines when pain is steadily improving and you do not need breakthrough doses.
Reduce in this order:
Stop the breakthrough strong pain medicine first (for example tapentadol/Temgesic).
Stop the anti-inflammatory medicine next.
Reduce paracetamol last.
If pain flares, step up one level for a day and then reduce again.
If you still need strong pain medicine beyond about 10–14 days, contact your surgeon or GP.